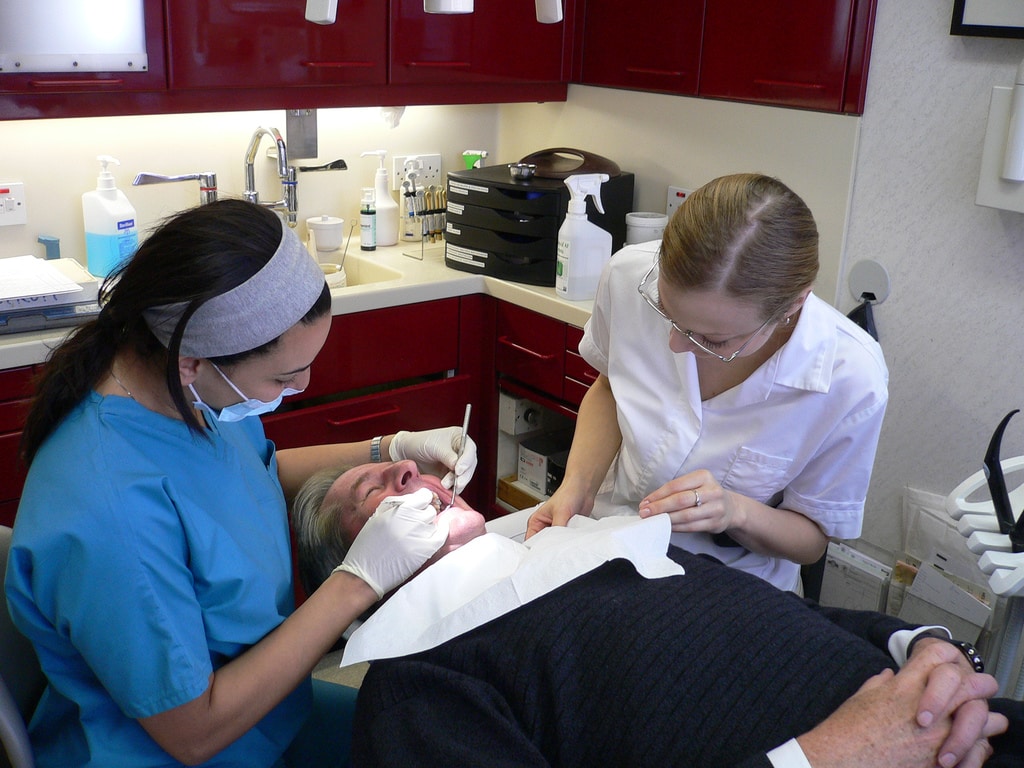
Tooth extraction is a common procedure that can be used to resolve a number of pressing dental problems. Often associated with the removal of badly decayed teeth, extraction is also the preferred option in a number of other circumstances. If you’d like a general overview, you can also read our detailed guide on what is tooth extraction.
Although some people are concerned about undergoing a tooth extraction, the reality is that contemporary dentistry techniques and highly effective painkillers result in the process being quick, painless and extremely safe.
We’ve taken a look at the various conditions which may result in extraction, as well as the process, so that you’ll know exactly what to expect.
Common Conditions that Require Tooth Extraction Treatment
A badly decayed tooth is often a prime candidate for extraction. In many cases, more conservative treatments such as dental fillings or root canal therapy may already have been tried but proved insufficient to stop the decay.
Not only are decayed teeth extremely painful, but if left untreated, bacteria can spread and affect overall health. Maintaining good oral hygiene and regular check-ups can significantly reduce these risks, which we discuss further in our article on the benefits of maintaining a regular dental check-up.
In some cases, removal may be recommended for individuals who have a compromised immune system (for example through an auto-immune condition or cancer treatment). For these patients, preventative extractions where only a moderate amount of decay is present are commonplace.
[elementor-template id=”1268″]
Over Crowded or Misaligned Teeth
Particularly in younger patients, it can be the case that there just isn’t enough room in the jaw bone for all the teeth. This can lead to newer teeth being unable to come through (erupt), or teeth being pushed into growing crookedly.
Although the teeth being removed are healthy, if they stay in place they are likely to cause significant problems. Healthy teeth may also be removed if gum disease (periodontal disease) is present. Gum disease can cause teeth to become loosened; removal is needed to minimise the risk of future problems.
Impacted wisdom Teeth
Wisdom teeth are the large molars at the back of the mouth that grow in during the late teens or early twenties. Impacted wisdom teeth are ones that don’t have sufficient space to come through properly or have emerged, but have come through awkwardly. Learn more about managing this issue in our guide on how to avoid an infection after wisdom teeth removal.
If left untreated, badly placed wisdom teeth can cause complications such as damage to nearby teeth, a cyst, infection or crowding of the teeth that are already in position. Impacted wisdom teeth are a common problem and extraction is often recommended as the best treatment to resolve the issue.
What Can I expect when I go for a Tooth Extraction?
Prior to the tooth being extracted, your dentist will want to take a thorough medical history, as well as undertake some diagnostic testing (usually an X-ray) to gain a clear picture of what the extraction is likely to involve.
This helps them determine the most appropriate type of extraction to perform. You will need to make sure your dentist is aware of any pre-existing medical conditions that may compromise treatment – blood clotting disorders, immune problems or heart problems, for example, could all increase the risk of complications.
Every extraction carries a small risk of bacteria travelling from the extraction site into the bloodstream – although the body’s immune system usually copes with this easily, in high-risk patients, antibiotics may well need to be taken after the extraction to minimise the risk of sepsis. If you have concerns about pain, anxiety, or recovery, our team specialises in pain-free dentistry to ensure your comfort every step of the way.
Anesthesia
If you haven’t had a tooth extracted recently, you may not be aware just how sophisticated modern anesthesia can be. Simple extractions are normally carried out under local anesthetic, administered through an injection.
For more complex extractions (surgical extraction), the local anesthetic may be augmented by anesthesia through an IV line or a general anesthetic may be used instead. In all cases, you shouldn’t feel any pain at all.
When the procedure is a more invasive one, patients may be given steroids (to minimise swelling during and after the extraction). Patients who are likely to become agitated during an extraction may also be offered sedatives to help make the process as comfortable and stress-free as possible.
Simple Extractions and Surgical Extractions
A simple extraction is one which involves removal of an intact tooth. Once the anesthesia has taken effect, the dentist loosens the tooth using an elevator (a specialist dental instrument), then tugs it free with forceps.
In comparison, a surgical extraction is often required where the top of the tooth is missing (perhaps due to decay or trauma), or the tooth is buried deep in the gum tissue (an impacted wisdom tooth, for example, may be almost completely beneath the gum line).
During a surgical extraction, the dentist will slice away gum and bone tissue that surrounds the tooth, then remove it. In some cases, the tooth will be removed in several pieces.
What Can I Expect After an Extraction?
Once the tooth has been removed, the dentist will pack the area with gauze swabs until a blood clot has formed over the site of the extraction. If necessary, they will also put in a few soluble stitches.
If required, the dentist will prescribe antibiotics and also painkillers (usually anti-inflammatory such as Ibuprofen). Typically, any discomfort will subside within a few days. Patients who have had a surgical extraction may experience more severe swelling (as the process is more invasive); in these circumstances, ice packs can be applied. Generally, it’s wise to take things easy for at least 24-hours after an extraction.
Oral Health Dos and Don’ts During Recovery From an Extraction
Do:
- Keep brushing and flossing, except at the extraction site
- Eat softer foods, particularly in the first few days
- Use a pillow or two to elevate your head and neck.
Don’t
- Smoke
- Spit forcefully
What Should I Look Out For?
Tooth extraction is a very safe procedure, but it is still a surgical intervention, which means that occasionally there may be side effects or complications. You should contact your dentist (or emergency medical provider, depending on the severity of the symptoms) if:
- The extraction site continues to bleed or starts bleeding heavily again
- There is discharge from the extraction site
- Discomfort stays the same or gets worse
- Swelling does not begin to subside
- You experience nausea, vomiting, problems breathing and/or a high temperature.
Visit our Services page to learn more.